A study published in the New England Journal of Medicine made headlines this week by showing that palliative care for terminal cancer patients, meaning pain and stress reduction care, extended their lives more than conventional chemo and radiation alone, and more than aggressive cancer treatments. The study focused on lung cancer patients whose cancer had spread. On average, those with conventional care alone lived six to twelve months. Those with palliative care as well lived three months longer and reported better quality of life. This study is a strong indicator that stress and pain reduction have powerful benefits. For an alternative perspective on why these make a difference . . . and why another alternative treatment that might make a difference as well, here’s anti-aging expert, Dr. Ron Rosedale. We caution you that while Dr. Rosedale’s views are intriguing . . . they’re also controversial, and they are not a substitution for the advice of your medical doctor. Here’s Ron Rosedale:
Listen to Short Interview – Broadcast on KGNU (6 minutes)
That’s Ron Rosedale, discussing the New England Journal of Medicine study that indicates how, adding stress and pain reduction care to conventional care for terminal cancer patients adds to an extension of their life, and an improvement in the quality of their life.
Extended Version of the Interview
Listen to Extended Interview (25 Minutes)
RON ROSEDALE: One of the reasons given in the New England Journal of Medicine Study for the life extension is that palliative care reduced stress, reduced pain, and these may have allowed for improved immune system. But if you look at it in the bigger picture, what you’re seeing is that aggressive care, or more of the care that is considered conventional will make a person worse. And that begs the question, will conventional care make a person worse in the chronic diseases of aging. So is the typical conventional treatment of heart disease, diabetes, heart disease and other chronic diseases of aging worsening the underlying disease instead of improving it? And my answer would be yes.
It’s a sad statement and would raise a lot of eyebrows, but I’ve said it for quite some time that if Medicine did nothing to these chronic diseases of aging, if they didn’t treat them at all, I think they’d be better off, and I think that’s very sad.
In the cancer study on palliative care, what I think is being revealed is the underlying science that aggressive cancer feeds on glucose. It requires an anaerobic fuel because it outpaces the blood supply. It can’t allow itself enough fuel to multiply quickly, if it were to burn fat, so it is an obligate glucose burner when it’s multiplying fast. Just like a sprinter has to burn sugar when they’re running fast. When cancer cells are multiplying rapidly, they require glucose because glucose can be burned without oxygen.
 When someone’s under stress, whether it’s from pain or excessive use of anti-cancer drugs, or they’re just plain worrying, does that increase blood sugar levels in the body?
When someone’s under stress, whether it’s from pain or excessive use of anti-cancer drugs, or they’re just plain worrying, does that increase blood sugar levels in the body?
RON ROSEDALE: Exactly. The potential reasons why palliative care improved outcomes in cancer patients is because it lowered glucose. But the most impressive way to lower glucose is just to not eat it. And yet that is not part of standard medical care for cancer patients. It totally eludes me. It’s very well known that the most aggressive cancers have to burn sugar and yet they don’t tell people not to eat it. When we’re talking about sugar, we’re not just talking about white table sugar. We’re talking about potatoes and rice and bread, cereals, starches will almost immediately turn into glucose in the body, or at least within a few minutes in the body, and that will feed the cancer cells. More importantly, they’ll also up-regulate an important hormone well-known in diabetes, but which plays a critical role in everybody’s lives, and that’s insulin. Insulin itself is a growth factor, and when insulin is raised, it stimulates cells to multiply, and that just stimulates cancer. So two of the best ways to reduce both the risk of cancer and to treat cancer, are to keep glucose levels as low as possible, and insulin levels as low as possible. So not one at the expense of the other. So you don’t want to take drugs that raise insulin in order to lower blood sugar. The only way to lower glucose and insulin at the same time is through dietary approaches. And yet that’s not even on the radar in standard cancer therapy treatments.
Last year, there was a study done on laboratory animals where researchers gave them intermittent fasting, meaning on some days they were given less food than on other days. There was reduction in the breast cancer tumors that had been injected into the lab animals that were doing this intermittent fasting. This was a dietary change.
RON ROSEDALE: Intermittent fasting is a modality that has been looked at for caloric restriction and extension of life. Caloric restriction is a known way to increase lifespan in virtually all species of animals ever tested. You don’t have to restrict calories all the time. You can just greatly restrict calories every other day. When they talk about increasing lifespan, and biology of aging studies, it’s really analogous to reducing cancer because that’s what most lab animals die of. It’s been known for over 70 years that restricting calories of lab animals will increase their lifespan. And therefore reduce both incidence and progression of cancer. One of the things we know in the biology of aging is that when you keep insulin levels low, it reduces the growth factors that cancer cells require to multiply. The importance of glucose is exemplified by the fact that PET scans all over the world are used to diagnose cancer, and they work by identifying areas of high glucose metabolism, and yet they still don’t people on a low glucose, low non-fiber carbohydrate, meaning starchy and sugary, diet.
It is not a disease that I would say I specialize in but I have treated cancer patients and I put all of them on a low to moderate protein, very low carbohydrate, high beneficial fat diet and they’ve done extremely well and have reversed quite a few cases of so-called met static and so-called cancer. Some have been studied worldwide actually. One was the first known case of survival. I can’t say there’s a cure for cancer but certainly one can at least use the science we know of. But the problem is, there’s really no money in it.
Unfortunately, the modalities that generally get widely used are the ones that have income, and not just for greed—income for supposed medical studies that would then get published. In other words, a pharmaceutical company, or any large corporation is not going to spend 50 to 100 million dollars on a treatment modality where they aren’t going to get any money back. So many of these treatments never get publicized because there aren’t good studies to back them. There are some animal studies because those are cheaper.
In India, I spent a couple of years in India for their diabetic problem, their heart disease problems. But I also wanted to look at cancer. There was a hospital that wished to do it, and they had accepted the dietary approach and wished to do it, but they said it can only be done in conjunction with standard therapy. Because otherwise it would never pass the ethics committee.
What I wanted to do is just test two groups of patients. Even two groups of patients where they were considered to be very terminal, which essentially means they had nothing to lose, and compare a dietary approach to a standard or aggressive chemotherapy approach. And that wasn’t passed. They wouldn’t allow that. They would only allow it in conjunction with chemotherapy, but that would have messed it up.
Is your concern that if you gave a dietary approach to slow down cancer growth and added chemotherapy, they would be fighting each other?
RON ROSEDALE: Yes. I think the adverse effect of the chemotherapy would really overwhelm some of the beneficial things you would see from the dietary approach. One of the major endeavors really in anybody who is sick in any way is to enhance the functioning of the immune system, and chemotherapy in a devastating manner impairs the function of the immune system. It almost seals many people’s death, when they have cancer. You will never, no matter what treatment you use, whether chemotherapy or radiation, wipe out all the cancer cells. There will always be some left over. Your immune system has to mop up the remainder. And you require a powerful immune system, and the chemotherapy really wipes out the immune system, so you don’t have that capability.
Even if you, through chemotherapy or radiation, kill 98% of the cancer, which would be largely unachievable in metastatic tumors, the other 2% will come back because you don’t have an immune system that would be able to take care of the rest. Whereas with a dietary approach, you increase the functioning of the immune system, and it’s one of the major ways it works, and it’s one of the major ways it extends lifespan in laboratory animals, is by improving the functioning of the immune system, which is what has to happen whenever someone is diseased, but especially, when someone has cancer.
In 2008, there were some startling studies about breast cancer and how women who had mammograms more frequently also had cancer diagnosed more frequently. Researchers concluded that in women who have less frequent mammograms, some of the tumors that would have been treated, if they were getting mammograms, are taken care of spontaneously by their bodies.
RON ROSEDALE: Yes, and there have been a lot of verifying studies that everybody gets cancer. Cancer cells develop in everybody most of the time. As long as you have a healthy immune system, it will recognize the cancer and eat it up. Also we’ve talked about the importance of proper signaling between the 20 billion cells that make us up. These signals are mediated mostly through hormones, and quite a few studies have shown that when insulin is kept low, the risk of breast cancer and prostate cancer and several other cancers is very much minimized. They’ve even shown that you can treat prostate cancer by lowering insulin and by inference, by lowering glucose.
There are studies that show these results. They’re not that rare, and I remember a study that showed that women who ate the least amount of pasta, and therefore, had a lower glucose load, had a lower incidence of breast cancer, and I believe that study was done in Italy. So there are studies that show these correlations at the very least between glucose, insulin and cancer, for both treatment and prevention. But unfortunately, it’s not commonly used, and it wouldn’t cost anything, and I strongly believe it’s the most powerful defense we have against both the risk of cancer and to treat cancer.
Right now, you’re talking about dietary approaches to treating cancer. The New England Journal of Medicine report regarding palliative care was looking more at how reducing stress can help the body, but you’re saying the mechanism might be similar – that by reducing stress, you reduce the kind of hormones and high blood sugars that can feed cancer.
RON ROSEDALE: For the same reason that when you reduce stress, you reduce epinephrine and nonepinephrin and corrison. Your body worries about living the next five minutes. If you’re going into battle with a lion, you’d like those hormones to enhance your fighting performance or your running performance. You don’t want the extra sugar. You’re not really going to be burning it. The article also talked about painkillers. Palliative care is essentially about reducing pain. When researchers gave people pain reduction medications in earlier studies, they seemed to have an enhanced survival. A plausible explanation is that also reduces blood sugar. Pain is a very powerful stress, and we know that when a person is under pain it will increase epinephrine, norepinephrine and other hormones. Any diabetic will tell you when they have pain, their blood sugar goes up. That’s certainly something I’ve seen in my patients for decades.
In your estimation it might be a wise choice for someone to take the gamble of focusing on noninvasive treatments such as reducing stress levels and changing their diet as a way to deal with cancer. But just as in India, medical ethics committees challenged you about using a dietary approach alone to treat cancer, without chemotherapy, people would probably be challenged in the United States for trying your approach. Especially for a disease such as small cell lung cancer, which was the focus of this palliative care study. The reason that conventional care is chosen so often is that the survival rate for metastasized small cell lung cancer, WITHOUT conventional chemotherapy and radiation, the average survival was two to three months. Whereas the average survival with chemotherapy and radiation is six months to a year. Statistics seem to make it very evident that conventional chemotherapy and radiation extends the life of someone with small cell lung cancer that has metastacized.
RON ROSEDALE: First of all, and this is what becomes so difficult now, there are so many studies that have been shown, subsequently to be false. When there is lots of money to be made, there is lots of incentive for drug companies to skew statistics in their favor. I think that’s now being brought before congress with Avandia. But we’ve seen it with many, many other drugs. Chemotherapy is very expensive. It makes lots of money for drug companies. So can you believe the statistics? My answer is I don’t know. Number two, what I feel might happen is that chemotherapy might extend certain people’s lifespan, but it also might sign their death certificate. In other words, it might extend your life a couple of months, but it will assure you die afterwards, because you won’t have an immune system. And that’s not looked at. Negative statistics will never get published. There’s no mandate to publish negative results like that. If it did occur, any drug company would hide it, and you’d never see that. So it’s really hard to tease fact from fiction in a lot of these studies. All you can do is go much deeper into the basic science of it. And understand that glucose feeds cancer, insulin is a signal for cells to multiply. Leptin plays a role. All of these are dietary signals. And then we have other pathways that involve protein that are very powerful d cancer progression, so much so that pharmaceutical companies are looking for ways to manipulate these pathways with drugs, even though we can do that just with what people eat, but there’s no money in that. So, it’s a problem.
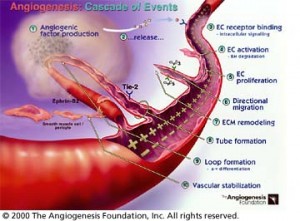 Before we close of the day, how about if we talk about related topic regarding cancer that might tie in with this discussion? Angiogenesis is a big word right now. Lots of people are interested in what can reduce the chance of angiogenesis is in cancer. Do you want to explain what angiogenesis is and how a dietary change might affect that?
Before we close of the day, how about if we talk about related topic regarding cancer that might tie in with this discussion? Angiogenesis is a big word right now. Lots of people are interested in what can reduce the chance of angiogenesis is in cancer. Do you want to explain what angiogenesis is and how a dietary change might affect that?
RON ROSEDALE: Angiogenesis literally means to build blood vessels, and it takes a lot of fuel for cancer cells to multiply, just as it takes more fuel for pregnant women to make a baby, and the fuel has to be transported through the bloodstream. For cancer cells to be able to multiply the body has to deliver the nutrients for the multiplications. That’s going to be through blood vessels, so cancer cells put out signals to build blood vessel into the tumor to feed itself. There are inhibitors of that blood building process that have been shown to reduce the growth of cancer.
But there’s another way one can look at it, too. What is it that the cancer cells are getting delivered? The major nutrients that cancer cells need delivered are going to be glucose and protein, and there are signals we know also that are required for angiogenesis. One of those would be insulin. Also leptin. And if a person eats too much protein, that will increase a pathway known as MTOR that will increase cell multiplication. It doesn’t take a big leap of faith or leap of science to just want to not deliver those nutrients to a cancer cell in your diet.
There are only two fuels your body can burn. This is major. You can only burn sugar or fat. Or byproducts of fat metabolism called ketones. And that’s it. You don’t have any other choice of fuel. And all of your cells in your body would actually much prefer to burn fat or ketones than glucose, with a few exceptions, with red blood cells being the major one. Whereas, cancer much prefers glucose. So that’s a major difference between cancer cells and healthy cells in your body. That difference has to be made use of, because there aren’t a lot of differences otherwise.
Cancer cells are regular human cells. They’re just healthy cells that have reverted back to their bacterial heritage that is telling them to multiply. They require the same nutrients that the rest of your cells require, with that one big difference. And that is, they prefer glucose and the rest of your cells essentially prefer fat. You have to utilize that difference. Don’t eat glucose. It’s as simple as that. The minimum daily requirement for glucose or any sugar and that means starch consumption is zero. You don’t have to have any. And if I had cancer, my intake of sugars and starches would be zero. That doesn’t mean you’d get your blood sugar down to zero. But you don’t have to give cancer cells any more sugar than your body would otherwise make. I also would not eat excess protein. You have to eat some because protein is an essential nutrient and otherwise you would die. I would eat lots of fats and good fats and fish oils. And I would eat coconut oil, olive oil, nuts, avocados. I would eat the fuel that the rest of your body would really be happy to burn and that cancer cells can’t use. We know that low levels of both of those hormones are associated with a very low risk of cancer. And an extension of lifespan otherwise. You’ll increase maintenance and repair.
Would also hang out with good friends and go for walks in the park and smell the flowers?
RON ROSEDALE: That sounds like a great idea. I most certainly would do that.







2 comments for “Cancer, Pain Relief & Diet: Ron Rosedale”